
It is summer here but the viruses and nasties are still in the air. The fact that quite a few children we know are currently fighting a tummy virus and vomiting, keeps me on my toes.
When you are a parent of a child with diabetes, you need to be well prepared for sick days. I decided to go over my sick day supplies and routines, just in case.
In the past 6 years we have been besieged by a number of viruses, sniffles, sore throats, coughs, ear infections, and three viral gastros that landed Mr T on a drip in hospital. Naturally, I have to have different plans for various degrees of sickness:
The "I do not feel well, but I am able to play" day(s)
BG’s high, Mr T a bit run down and tired, maybe runny nose or a bit of a cough, usually caused by a virus, but still enough energy to play and eat properly.
Plan:
Keep checking BG more often the usual (two hourly), keep correcting the high BG’s. Check for ketones, if none recheck after 2 consecutive high BG readings. Lots of fluids, treat the illness, food and INSULIN, regularly. If two consecutive BG readings are high and I have eliminated all of the other usual suspects (see this link HERE ), I suspect temporary insulin resistance due to the virus and I consider using an increased TEMPORARY BASAL in consultation with our DE. I am so glad our DE is just on the other end of the line when I need him. It makes sense to me: the resistance to insulin is there, therefore both needs for bolus and basal become greater, temporarily.
The: "I feel really sick and I need Antibiotic" day(s)

If it comes to antibiotics, I know Mr T’s numbers are going to be really stubborn for a few days. I have notice a trend where insulin resistance occurs as soon as antibiotics are taken but almost normal sensitivity to insulin comes back just before the time of the next dose approaches.
Plan:
Temp basal up, and as above, frequent BG testing, testing for ketones, lots of fluids, AB and soft food to ensure food gets eaten even if the throat hurts. Having carbs free food ready is always good for the times when the BG is high, correction is given and Mr T is hungry. Eating carbs free food should not increase the BG further.
I know I need to be very, very careful with the changes to insulin doses, especially when increasing them, since the sensitivity can come back and catch me unprepared, driving Mr T’s BG lower then desired.
The dreaded: "I am vomiting and I can not stop it" day(s)

You will know them, there is no doubt. Vomiting of any sorts and for any reason is one symptom I dread. I do not mind Mr T hanging around other kids with sniffles, but I do keep him far away from anybody vomiting.
I have explained to the teacher the consequences of Mr T catching gastro – usually this means a drip in a hospital. I have asked her to inform me if there are any cases in the class so that I can keep a closer eye on him, or even take him out of school for a day or two.
Plan: One off vomiting is not a big deal, but if he can not keep the fluids including carbs and/or a bit of food down, I have to be careful with insulin dosing for fear of him going too low and then not being able to get his BG up via adding carbs orally. In this case, or if vomiting persists I contact the DE and the Pediatrician, with a forewarning that we may need a drip. In these instances only a drip can ensure that there is enough glucose and fluid intake (that will not be ejected via vomiting) to allow the necessary insulin to be given which in turn will prevent the development of ketones.
What about ketones?
Ketones are too important and too dangerous to talk about them in passing so I’ll dedicate a post just to them. Promise.
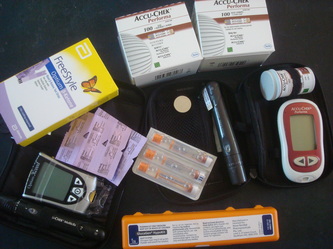
My "sick day kit" inventory
* Extra blood glucose testing strips,
* Spare batteries for blood glucose meters,
* Ketone testing strips (blood or urine testing ones),
* Glucagon,
* Your DE and Doctors contact details.
It gives me piece of mind knowing I have these spares handy if needed, rather then going to get them with a vomiting child in tow.
However, I do hope I will not need them any time soon. Wishing you the same.


 RSS Feed
RSS Feed
